National and International Programmatic Perspective on Facilitators and Barriers for Sudan's Health Sector Response on Female Genital Mutilation (2016-2018): A Qualitative Study
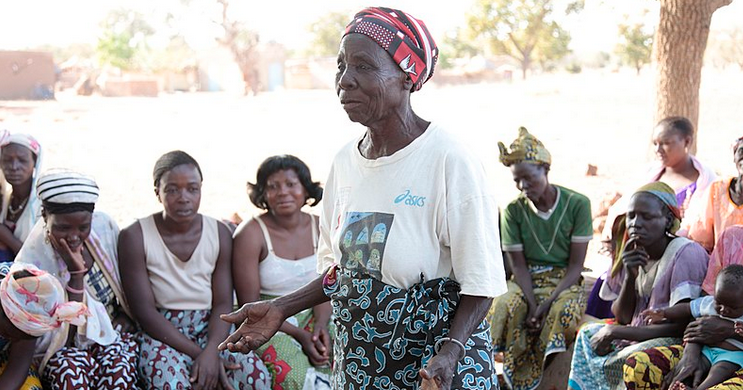
"Understanding the factors affecting planning and implementation of Sudan's health programme addressing FGM may potentially mitigate barriers and improve results."
The national female genital mutilation (FGM) abandonment strategy in Sudan is multisectoral and coordinated by a national taskforce led by the Ministry of Welfare and Social Security (MoWSS). The health sector played a minimal role until 2016, when it was included in the Sudan Free From Female Genital Cutting (SFFGC) programme. The emphasis was mainly on midwives, as they are the main driving force in FGM medicalisation in Sudan, where 64% of women (15-49 years) with FGM have had it performed by midwives. Between 2016 and 2018, Sudan had significant achievements in the health component of SFFGC programme, prompting this study to understand how and why this success occurred.
The health interventions funded by the SFFGC programme were guided by the World Health Organization (WHO)'s 4 pillars of action: strengthen governance and funding (pillar 1); increase health workers' knowledge and skills (pillar 2); improve monitoring and evaluation (M&E) and accountability (pillar 3); and create a supportive environment (pillar 4). The study used these 4 pillars to categorise the reported scope of the health plan and activities. In addition, the Consolidated Framework for Implementation Research (CFIR) informed the interview guide and data analysis. In brief, CFIR has 5 domains with a total of 39 constructs: (i) intervention characteristics; (ii) outer setting; (iii) inner setting; (iv) characteristics of the individuals; and (v) process. The researchers adapted the 5 domains and 12 of its constructs to align with Sudan's context.
Eight Sudanese and 2 international programme managers representing governmental, international, and national organisations and donor agencies participated in interviews. Their job positions required detailed involvement in planning, implementing, and evaluating diverse health interventions in the areas of the 4 WHO pillars of action. Select findings:
- Respondents' reported activities for strengthening governance and finance (pillar 1) included conducting multi-sectoral national or state-level advocacy, championing integration of FGM, developing health sector plans, and establishing various technical and multisectoral coordination committees at national and state level.
- With respect to activities in strengthening knowledge and skills of health workers (pillar 2), respondents mentioned the development of national guidelines on FGM management, social norm change training modules, and the rollout of FGM content in pre-service and in-service trainings to diverse health professionals. For instance, medical students engaged their peers through the SCORAtalk, akin to "TEDx talks", which were set up to relay FGM-related messages in different art forms such as music, plays, and poetry to 8,650 medical students who attended the event, either in-person or virtually.
- Respondents cited several activities that aimed to strengthen M&E and accountability (pillar 3), such as involvement in generating data on FGM-related knowledge, attitudes, and practices among diverse health professionals and traditional birth attendants.
- Respondents' cited activities that contributed to creating a supportive environment (pillar 4) mainly reached out to health professions and students through awareness raising, social norm change trainings, and change agents' activities that resulted in public declarations against FGM and calls for a law, and the development of FGM content within the primary school health manual.
Respondents identified funding availability and comprehensive plans, integration of FGM-related interventions within existing priority health intervention packages, and presence of an evaluation and feedback culture within international organisations as implementation facilitators. Furthermore, respondents reported that the continuous championing and advocacy on the part of international non-governmental and governmental agencies (INGGA) facilitated the uptake of FGM as a public health issue.
The barriers were low health system functionality, low inter-organisational coordination culture, power asymmetries in decision-making during planning and implementation of nationally and internationally funded interventions, and non-supportive attitudes among health workers. Respondents felt that the external design of some SFFGC-related research activity lacked depth in contextual understanding. One of them said, "The experts who were brought... had the mindset of foreigners not the mindset of Sudanese....Despite the sensitivity on FGM they talked about artists and musicians as ambassadors for change...they were far from the reality of Sudan, because [FGM has] … additional sensitivity [being] related to reproductive health which is highly sensitive [and requires a credible and trustworthy role models, e.g., health workers to act as change agents." There was a sense that health topics related to societal norms were also not prioritised in general, possibly because senior governmental programme managers recognise that such complexity that would be onerous to multiple sectors' systems with limited functionality and coordination.
Among the suggestions offered based on the findings:
- Engage health professionals, clients, and FGM survivors, as well as national non-governmental organisations (NNGOs) and relevant legal and social sectors in stopping FGM medicalisation and in improving quality of services. Studying the impact of these stakeholders' involvement would add to the existing limited body of evidence.
- Foster a change in attitudinal stances among midwives and the society at large as a prerequisite for anti-FGM laws and policies to be successfully enacted and followed.
- Address raising employment and pay levels for midwives in order to reduce monetary incentives for performing FGM.
- Capture additional insights from health service users and beneficiaries after states and localities implement SFFGC activities to scale.
In conclusion, interventions to "change midwives' supportive values and attitudes towards FGM, ...strengthen joint accountability, address power equity in decision-making and strengthen participatory engagement and intersectoral and multisectoral coordination would need to be considered in future programming."
BMJ Open 2023;13:e070138. doi:10.1136/bmjopen-2022-070138 - sent from Wisal Ahmed to The Communication Initiative on July 12 2023. Image caption/credit: A traditional midwife tells her stories of childbirth at a community discussion about female genital mutilation/cutting (FGM/C). "When we heard there were no benefits to cutting from the peer educators, it reinforced what we already knew," she says. Jessica Lea/DFID via Wikimedia (CC BY 2.0 Deed)
- Log in to post comments












































